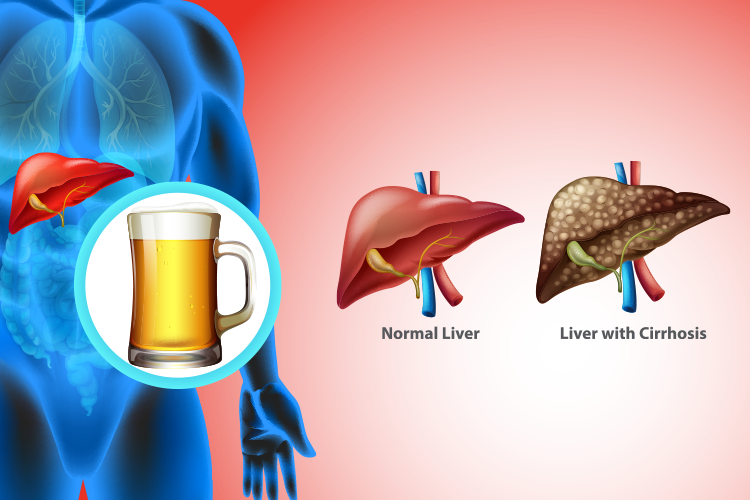
Alcoholic Liver Disease
Alcoholic Liver Disease (ALD) is a serious condition caused by long-term and excessive alcohol consumption. The liver is responsible for processing and breaking down alcohol, but when drinking becomes excessive, it overwhelms the liver, leading to fat buildup, inflammation, and scarring. Over time, this can progress to life-threatening conditions such as cirrhosis or liver failure. This article explains everything you need to know about alcoholic liver disease, including its causes, stages, symptoms, diagnosis, treatment, and prevention.
Stages of Alcoholic Liver Disease
- Alcoholic Fatty Liver (Steatosis): The earliest stage, where fat builds up in liver cells. Often reversible if alcohol consumption stops.
- Alcoholic Hepatitis: Involves liver inflammation, swelling, and damage to liver cells. Can cause symptoms such as jaundice, abdominal pain, and fever. May be mild, but in severe cases it can be life-threatening.
- Alcoholic Cirrhosis: The most advanced stage, where healthy liver tissue is replaced by scar tissue. Permanent damage that leads to reduced liver function. Can result in complications like portal hypertension, ascites, and liver cancer.
Causes of Alcoholic Liver Disease
- Amount and duration of alcohol intake – long-term heavy drinking is the biggest risk.
- Gender – women are more vulnerable to alcohol-induced liver damage than men.
- Genetics – family history may increase susceptibility.
- Obesity – increases the risk of liver inflammation.
- Nutritional deficiencies – poor diet worsens alcohol-related damage.
Symptoms of Alcoholic Liver Disease
- Fatigue and weakness
- Loss of appetite
- Nausea and vomiting
- Abdominal pain or discomfort
- Yellowing of skin and eyes (jaundice)
- Swelling in the abdomen (ascites)
- Confusion, memory loss, or difficulty concentrating (hepatic encephalopathy)
- Easy bruising and bleeding
Complications of Alcoholic Liver Disease
- Portal Hypertension – high blood pressure in the veins of the liver.
- Esophageal Varices – enlarged veins that may rupture and bleed.
- Ascites – fluid buildup in the abdomen.
- Liver Failure – inability of the liver to function properly.
- Hepatocellular Carcinoma (Liver Cancer).
Diagnosis of Alcoholic Liver Disease
- Medical history and alcohol use assessment
- Physical examination – checking for signs like jaundice or enlarged liver
- Blood tests – to measure liver enzymes (AST, ALT, bilirubin)
- Imaging tests – ultrasound, CT scan, or MRI to detect liver changes
- Liver biopsy – provides the most accurate diagnosis and assesses the extent of damage
Treatment for Alcoholic Liver Disease
- Complete alcohol abstinence – the most important step to prevent disease progression.
- Nutritional therapy – improving diet and treating vitamin deficiencies.
- Medications – steroids or other drugs to reduce liver inflammation in severe alcoholic hepatitis.
- Management of complications – controlling fluid buildup, bleeding, and infections.
- Liver transplant – in cases of end-stage liver disease when the liver can no longer function.
Diet and Lifestyle Recommendations
- Avoid all alcohol completely
- Eat a balanced diet rich in fruits, vegetables, and whole grains
- Include lean protein sources to support healing
- Take vitamin supplements (especially vitamin B and folic acid) if prescribed
- Stay physically active but avoid overexertion
- Get regular medical checkups to monitor liver health
Prevention of Alcoholic Liver Disease
- Drink in moderation if you consume alcohol.
- Eat a nutritious diet and maintain a healthy weight.
- Stay physically active.
- Get vaccinated against hepatitis A and B to protect your liver.
- Regularly monitor liver health if you have a history of heavy drinking.
Living with Alcoholic Liver Disease
Living with ALD requires lifestyle adjustments and medical guidance. Quitting alcohol can be difficult, but support groups, counseling, and rehabilitation programs can help. With early diagnosis and commitment to change, it is possible to halt or even reverse early stages of the disease.