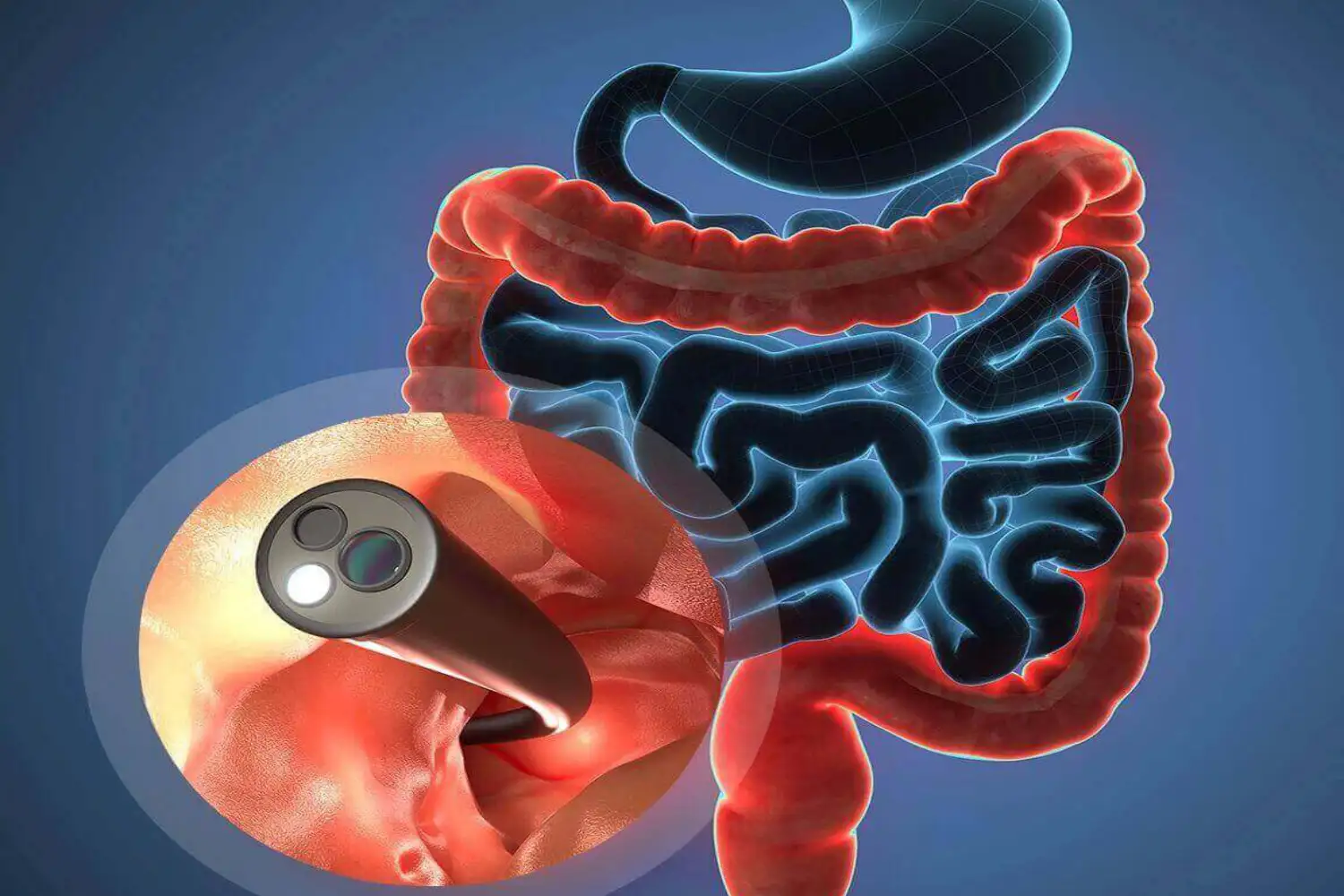
Colonoscopy
A colonoscopy involves the use of a long, flexible tube called a colonoscope. The instrument is inserted through the rectum and advanced through the colon. The camera at its tip allows the doctor to view the entire length of the colon on a screen.
In addition to diagnosis, a colonoscopy can also be therapeutic, allowing the removal of polyps, control of bleeding, and biopsy of suspicious tissue.
Why is a Colonoscopy Performed?
Doctors recommend colonoscopy for both screening and diagnostic purposes. Common reasons include:
- Screening for colorectal cancer – usually recommended from age 45 onward.
- Detection and removal of polyps – preventing cancer development.
- Investigation of gastrointestinal symptoms such as:
- Chronic diarrhea
- Rectal bleeding
- Unexplained abdominal pain
- Changes in bowel habits
- Unexplained weight loss or anemia
- Diagnosis of inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis.
- Monitoring patients with a history of polyps or colorectal cancer.
Preparation for Colonoscopy
Proper preparation is critical for a successful colonoscopy. A clean colon ensures the doctor has a clear view. The preparation usually involves:
- Bowel cleansing – Patients are asked to drink a prescribed laxative solution a day before the procedure.
- Clear liquid diet – Allowed fluids include water, broth, tea, apple juice, and clear sports drinks.
- Fasting – No solid food 6–8 hours before the test.
- Medication review – Patients should inform their doctor about blood thinners, diabetes medicines, or other drugs.
How is a Colonoscopy Performed?
The procedure usually takes 30–60 minutes and follows these steps:
- Sedation – Patients are given sedatives or anesthesia for comfort.
- Insertion of colonoscope – The doctor inserts the scope through the rectum and advances it slowly through the colon.
- Examination – The lining of the colon is carefully inspected for inflammation, ulcers, bleeding, polyps, or tumors.
- Biopsy or polyp removal – If abnormal tissue or polyps are found, they can be removed or biopsied immediately.
- Completion – The scope is withdrawn while the colon is re-examined.
Conditions Detected by Colonoscopy
Colonoscopy is considered the gold standard for diagnosing colon-related conditions. Some common findings include:
- Colorectal polyps
- Colon and rectal cancers
- Diverticulosis and diverticulitis
- Inflammatory bowel disease (Crohn’s, ulcerative colitis)
- Unexplained gastrointestinal bleeding
- Infections or ischemic colitis
Benefits of Colonoscopy
- Cancer prevention – Early removal of polyps reduces colorectal cancer risk.
- Accurate diagnosis – Direct visualization allows detection of even small lesions.
- Therapeutic use – Polyps can be removed, and bleeding controlled during the same procedure.
- Guided treatment – Biopsies help determine the exact cause of symptoms.
- Improved survival rates – Early detection of colon cancer significantly improves outcomes.
Risks and Complications
Although colonoscopy is generally safe, minor risks may include:
- Bloating or cramping after the procedure
- Bleeding at biopsy or polyp removal sites
- Perforation of the colon (very rare, <1 in 1000 cases)
- Reactions to sedatives
The overall risk is very low, especially when performed by experienced specialists.
Recovery and Aftercare
After the procedure:
- Patients are monitored until sedation wears off.
- A mild bloating or gas sensation may occur due to air introduced during the procedure.
- Normal diet can usually be resumed the same day.
- Driving is not allowed for 24 hours due to sedation.
- Any severe abdominal pain, fever, or heavy rectal bleeding should be reported immediately.
Colonoscopy vs. Other Screening Methods
- Fecal occult blood test (FOBT)
- Stool DNA tests
- CT colonography (virtual colonoscopy)
- Sigmoidoscopy
However, colonoscopy remains the most reliable since it allows both detection and treatment in one session.
When Should You Get a Colonoscopy?
- Average-risk individuals – Start at age 45, repeat every 10 years if normal.
- High-risk individuals – Those with a family history of colorectal cancer, polyps, or genetic syndromes may need earlier and more frequent screening.
- Symptomatic patients – Any unexplained rectal bleeding, persistent changes in bowel habits, or unexplained anemia warrants an immediate evaluation.