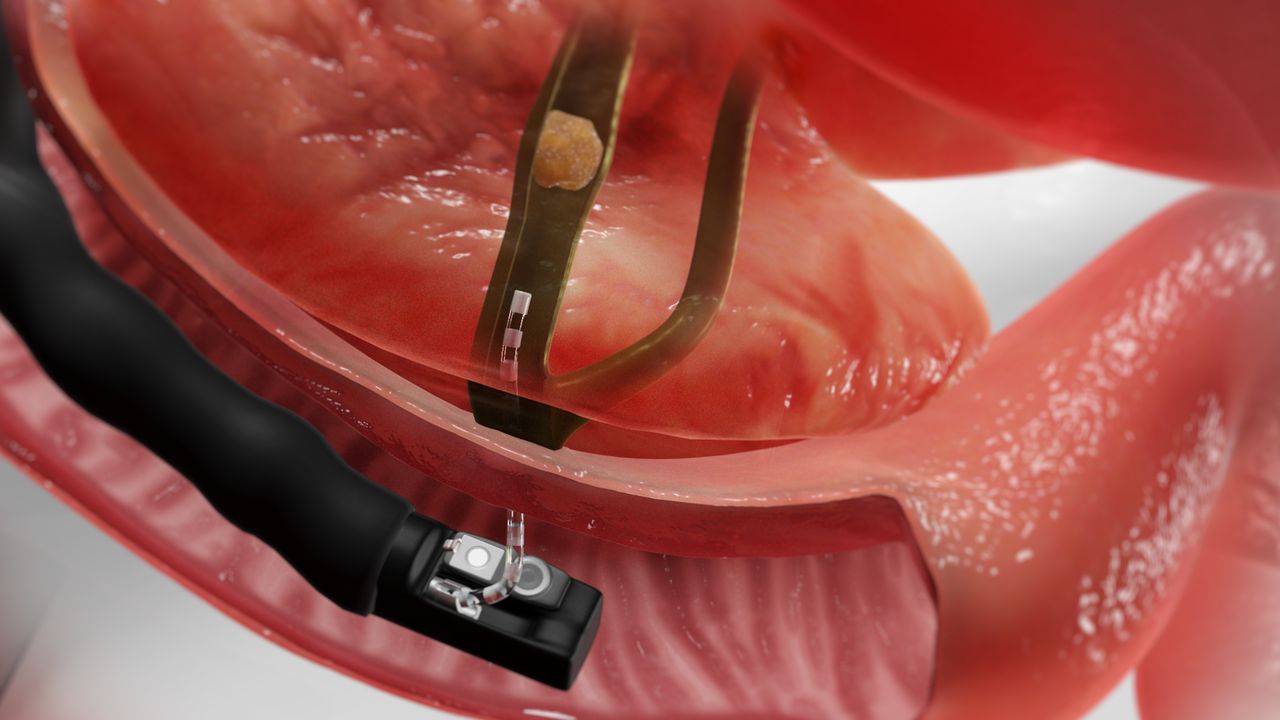
ERCP
Endoscopic Retrograde Cholangiopancreatography, widely known as ERCP, is a medical procedure that plays a crucial role in diagnosing and treating conditions related to the bile ducts, gallbladder, pancreas, and liver. Unlike ordinary diagnostic scans, ERCP combines endoscopy and fluoroscopy to both identify problems and provide immediate treatment in the same session.
It is a highly specialized technique performed by gastroenterologists with expertise in advanced endoscopy. Since ERCP can both diagnose and treat conditions, it often reduces the need for multiple hospital visits or surgeries.
Why ERCP Is Performed
ERCP is often recommended for patients with symptoms or test results that suggest problems in the bile or pancreatic ducts. Common reasons for undergoing ERCP include:
- Gallstones in the bile duct: Stones may block the flow of bile, causing jaundice, infection, or severe pain.
- Bile duct narrowing (strictures): Often caused by scarring, tumors, or inflammation.
- Pancreatic duct issues: Such as strictures, stones, or leaks leading to recurrent pancreatitis.
- Tumors or cancers: ERCP helps in diagnosing and managing cancers of the bile ducts, pancreas, or gallbladder.
- Bile or pancreatic fluid leaks: These may occur after injury or surgery and require immediate management.
By identifying and treating these issues in one session, ERCP provides both relief and diagnostic clarity.
How ERCP Works
The ERCP procedure combines two techniques:
- Endoscopy: A thin, flexible tube with a camera (endoscope) is passed through the mouth, esophagus, and stomach into the duodenum.
- Fluoroscopy (X-ray imaging): A contrast dye is injected into the bile and pancreatic ducts. This dye makes the ducts visible on X-ray, helping the doctor identify blockages, strictures, or stones.
If abnormalities are found, the gastroenterologist can:
- Remove gallstones from the ducts.
- Insert stents to keep ducts open.
- Perform a sphincterotomy (cutting the muscle at the duct’s opening) to improve drainage.
- Take biopsies for suspected cancer or infection.
Preparation for ERCP
Proper preparation is vital to reduce risks and ensure success. Patients are usually instructed to:
- Fasting: Avoid eating or drinking for 6–8 hours before the procedure.
- Medication adjustments: Stop or adjust blood thinners, diabetes medicines, or other drugs if advised.
- Inform doctors: Provide details about allergies, pregnancy, or previous reactions to sedation.
- Arrange transport: Sedation or anesthesia is given, so patients cannot drive after the procedure.
Step-by-Step Procedure
- Sedation: Most patients receive conscious sedation or general anesthesia for comfort.
- Endoscope insertion: The doctor guides the endoscope into the digestive tract.
- Dye injection: A small catheter delivers contrast dye into the bile or pancreatic ducts.
- X-ray imaging: Fluoroscopy detects stones, strictures, or other problems.
- Therapeutic intervention: Stones may be removed, ducts widened, or stents inserted.
- Completion: The endoscope is carefully withdrawn once treatment is complete.
The entire process usually takes between 30 and 90 minutes.
Risks and Complications
Although ERCP is safe in experienced hands, it does carry risks, including:
- Pancreatitis: The most common complication, with abdominal pain and digestive issues.
- Infections: Such as cholangitis, an infection of the bile ducts.
- Bleeding: May occur after sphincterotomy or biopsy.
- Perforation: A rare but serious risk involving a tear in the digestive tract.
- Sedation-related issues: Breathing or heart complications in sensitive patients.
To reduce risks, ERCP is performed only when strongly indicated and by skilled specialists.
Recovery After ERCP
- Resting: Patients should avoid strenuous activities for 24 hours.
- Hydration: Drinking fluids once fully awake helps with recovery.
- Diet: Light meals are usually recommended initially.
- Symptom monitoring: Mild sore throat, bloating, or nausea may occur but usually resolve quickly.
Patients should contact their doctor immediately if they experience severe abdominal pain, fever, vomiting, or jaundice. These may indicate complications.
Alternatives to ERCP
While ERCP is unique because it allows both diagnosis and treatment, some non-invasive alternatives are available:
- Magnetic Resonance Cholangiopancreatography (MRCP): Uses MRI imaging for a detailed view of bile and pancreatic ducts.
- Endoscopic Ultrasound (EUS): Combines endoscopy with ultrasound to evaluate ductal and surrounding structures.
Both are excellent for diagnosis but cannot provide immediate treatment like ERCP.
Advantages of ERCP
- Combines diagnosis and treatment in one procedure.
- Prevents complications like infections or jaundice caused by duct blockages.
- Reduces the need for invasive surgeries.
- Provides quick relief from painful symptoms.
Who Should Avoid ERCP?
- Patients with uncontrolled bleeding disorders.
- Individuals allergic to contrast dye.
- Patients with severe cardiopulmonary problems.
- Those who can be managed effectively with less invasive alternatives like MRCP.
The doctor carefully evaluates risks before recommending ERCP.
Living After ERCP
For many patients, ERCP significantly improves quality of life. By removing stones, widening narrowed ducts, or treating leaks, it relieves pain, reduces jaundice, and prevents repeated hospital visits.
Lifestyle adjustments also play a role in recovery and long-term health. Eating a balanced diet, limiting alcohol, maintaining a healthy weight, and following medical advice can reduce the risk of recurrent biliary or pancreatic issues.